Prenatal screening saw many huge changes in the recent decade, thanks to recent technologies that examine fetal DNA from a mother’s sample of blood.
What exactly is cell-free fetal DNA?
Cell-free fetal DNA contains microscopic pieces of DNA from placental cells that escape into the mother’s circulation when the placenta ruptures. You can detect them as early as the 6 weeks of pregnancy, but it is best to wait until the 10th week when concentrations are high enough to warrant testing. It is around 150 base pairs in length, which is significantly smaller than the body’s cell-free DNA. This scientific accomplishment represents a watershed moment in prenatal screening.
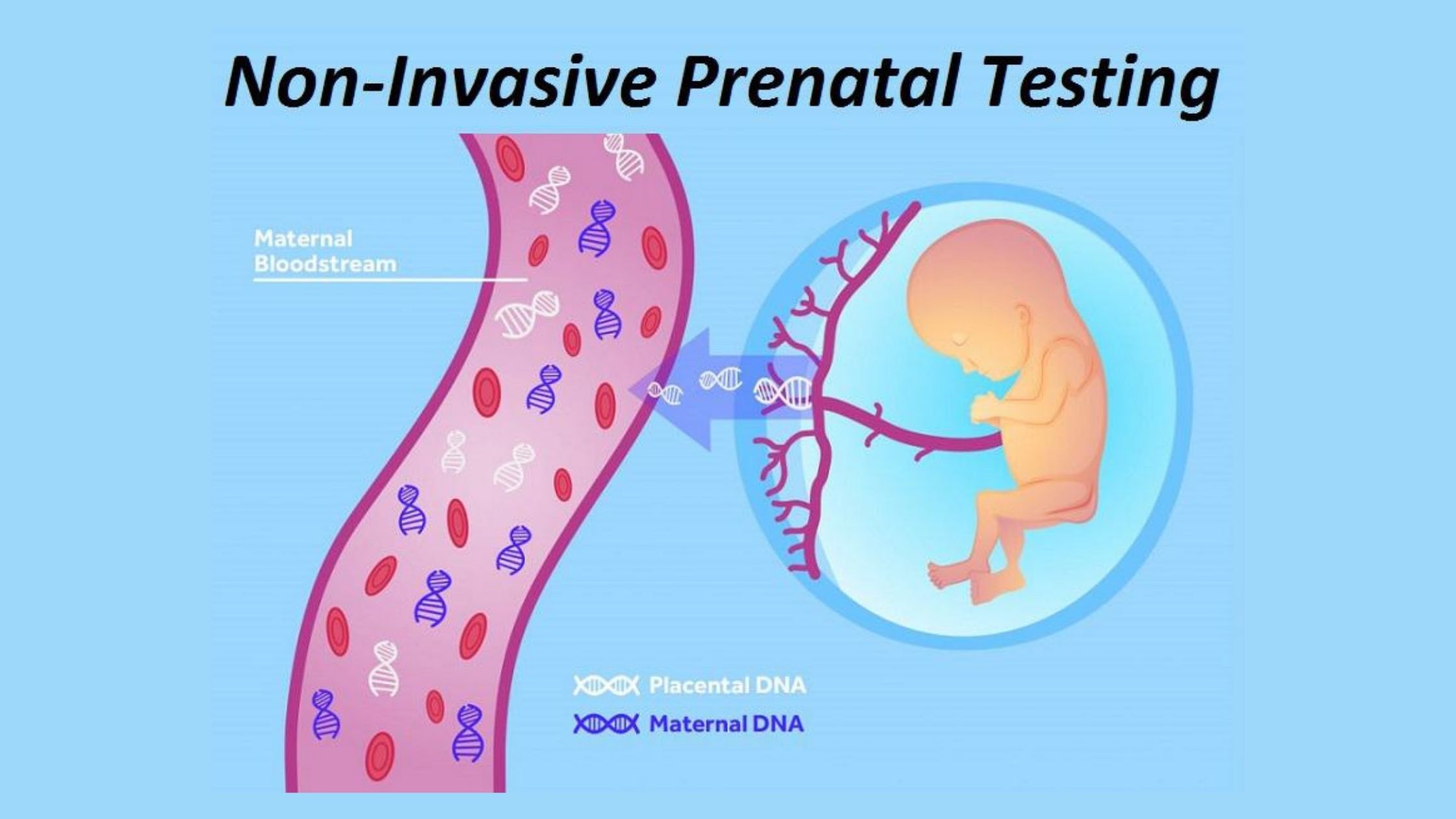
Non-invasive prenatal testing and fetal DNA
Non-invasive prenatal testing (NIPT) has transformed the diagnosis of prenatal genetic disorders.
NIPT tests examine the cell-free DNA in an expectant woman’s blood, which contains both fetal and maternal DNA, using NGS sequencing technology. This method enables us to detect the following aneuploidy:
- Trisomy occurs when there are 3 duplicates of a chromosome rather than the typical two.
- Monosomy occurs when one of the two copies of a chromosome is missing.
- A microdeletion occurs when a small piece of a chromosome is missing.
Because of the large variety of NIPT tests available on the market, it might be challenging for people to choose the most appropriate test for their scenario.

Some tests, for example, look for aneuploidy or other less prevalent trisomies. Your doctor should be able to advise you on the best option for you.
Why NIPT is so popular?
Foetal DNA-based testing offers a detection probability of 99 percent or higher, with a false positive rate of less than 0.1 percent, reducing the number of women who undergo unnecessarily invasive tests to one in 1,000. In short, such tests make up a huge advancement infrequent genetic disease detection methods (trisomies 21, 18, and 13) and have spread to many national health care systems as a result.



Leave a Reply
Your email is safe with us.